6 Safe Home Remedies for Baby Gas
Watching your precious little one squirm, cry, and fuss due to gas pain can be heartbreaking for any parent. It’s a common yet distressing issue for newborns and infants, whose tiny digestive systems are still learning the ropes. You’re not alone in feeling helpless, but the good news is there are several safe, gentle, and effective home remedies you can try to bring your baby comfort and peace.
This article will guide you through six tried-and-true methods to help relieve your baby’s gas, offering practical advice and a supportive hand through this often challenging phase. Remember, every baby is unique, so what works for one might not work for another. Patience and observation are your best tools!
Understanding Baby Gas What Causes It
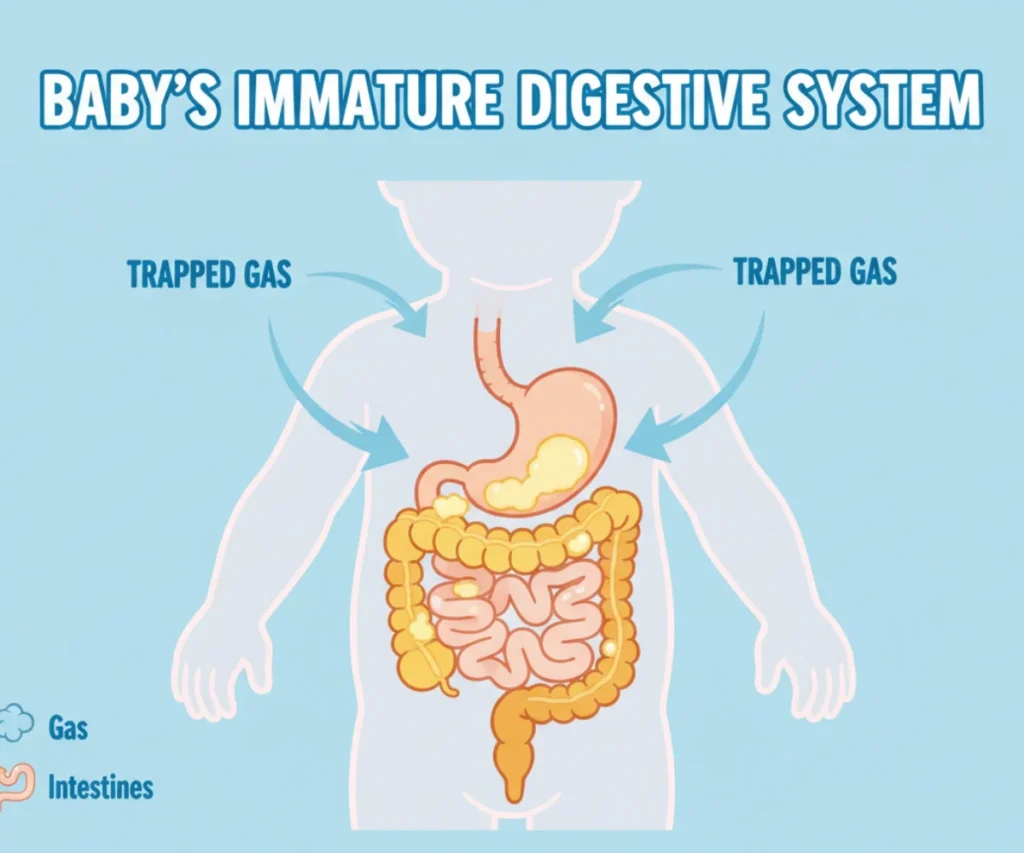
Before diving into remedies, it helps to understand why babies get gassy in the first place. Their digestive systems are incredibly immature, still developing the enzymes and gut flora needed to break down food efficiently. This makes them prone to swallowing air, especially during feeding or crying, which can lead to uncomfortable gas bubbles.
Common culprits include:
- Swallowing air during feeding: Whether breastfed or bottle-fed, babies can gulp air if their latch isn’t optimal, the bottle nipple flow is too fast, or they’re feeding in a less-than-ideal position.
- Immature digestive system: A baby’s gut is still learning to process food, sometimes leading to fermentation and gas production.
- Dietary factors: For breastfed babies, certain foods in the mother’s diet might occasionally contribute to gas, though this is often debated and varies greatly. For formula-fed babies, a sensitivity to a particular formula can be a factor.
- Rapid feeding: When babies eat too quickly, they tend to swallow more air.
Recognizing the signs of gas is key: fussiness, crying, pulling legs up to the chest, a hard or distended belly, and passing gas (sometimes with relief, sometimes not) are all common indicators.
1 Gentle Tummy Massage
A gentle tummy massage is often a parent’s first line of defense against baby gas. Not only does it help to move trapped gas through the digestive system, but it also offers a wonderful opportunity for bonding with your little one. The warmth of your hands and the rhythmic strokes can be incredibly soothing.
How to Perform a Tummy Massage for Gas Relief
Make sure your baby is calm, fed (but not immediately after a full meal), and in a warm, comfortable environment. Lay them on their back on a soft blanket or changing table.
- Warm Your Hands: Rub your hands together to warm them. You can also use a small amount of baby-safe lotion or oil (like unscented almond oil) to reduce friction and make the massage smoother.
- The “I Love U” Stroke: Imagine an “I” on your baby’s left side (downward stroke), an “L” across their belly from right to left and then down (like an inverted L), and a “U” beginning on the lower right, up, across, and down to the lower left (like an inverted U). This follows the natural path of digestion.
- Circular Motions: Gently rub their tummy in small, clockwise circular motions around the navel. Use the pads of your fingers, applying very light pressure.
- Knees to Belly: After a few minutes of massage, gently push your baby’s knees up towards their chest. Hold for a few seconds, then release. This compression can help release trapped gas. Repeat several times.
Tips for Success: Perform the massage when your baby is relaxed, not when they are actively crying or distressed from gas. Consistency is key; a short massage several times a day can be more effective than one long session.
2 Bicycle Legs and Tummy Time
Movement is a powerful ally in the fight against baby gas. Two simple yet effective techniques involve your baby’s legs and their tummy position: the bicycle legs exercise and regular tummy time.
Bicycle Legs Exercise
This classic remedy involves gently moving your baby’s legs in a pedaling motion, mimicking riding a bicycle. The movement helps to stimulate intestinal activity and physically push gas bubbles through their system.
- Position Your Baby: Lay your baby on their back on a flat, comfortable surface.
- Grasp Their Ankles: Gently hold your baby’s ankles or lower shins.
- Pedal Away: Slowly and gently move their legs as if they are pedaling a bicycle. Alternate bringing one knee up towards their tummy while extending the other leg.
- Gentle Pressure: You can also bring both knees gently towards their chest at the same time, holding for a few seconds before extending them.
Benefits: This exercise not only aids in gas relief but also strengthens your baby’s leg muscles and hip flexibility. Perform this when your baby is calm and receptive, perhaps after a diaper change or during playtime.
Tummy Time for Gas Relief
Tummy time is crucial for your baby’s development, strengthening neck and core muscles. It also provides gentle pressure on their abdomen, which can encourage gas to move and release.
- When to Do It: Introduce short sessions of tummy time (3-5 minutes) several times a day, especially when your baby is awake and alert, but not right after a feeding.
- How It Helps: The slight pressure on their belly helps to dislodge and expel gas.
- Making it Fun: Place interesting toys or a mirror in front of them to keep them engaged. Supervise your baby closely during tummy time.
3 Warm Bath Comfort
A warm bath can be a surprisingly effective and wonderfully soothing remedy for a gassy baby. The warmth of the water helps to relax abdominal muscles, which in turn can ease spasms and allow trapped gas to move more freely. Plus, the overall experience of a bath can be calming for both baby and parent, reducing stress that can sometimes exacerbate digestive upset.
How a Warm Bath Soothes Gas
- Muscle Relaxation: Just like a heating pad on an adult’s sore muscles, warm water helps to relax your baby’s tense belly muscles, providing comfort and potentially relieving cramps associated with gas.
- Distraction and Relaxation: The gentle immersion in warm water, the comforting touch of your hands, and the change of environment can distract your baby from their discomfort and promote overall relaxation, which can also aid digestion.
- Gentle Pressure: The water itself provides a mild, even pressure around your baby’s tummy, which can be similar to a light massage, encouraging gas bubbles to disperse.
Tips for a Gas-Relieving Bath
- Ensure Safety First: Always check the water temperature carefully using a bath thermometer (aim for 98-100°F or 37-38°C) or your elbow. The room should also be warm to prevent your baby from getting cold.
- Shallow Water: Fill the tub with just enough water to cover your baby’s tummy when they are lying down.
- Gentle Entry: Slowly lower your baby into the water, talking to them softly to keep them calm.
- Tummy Rub in Water: Once your baby is settled and enjoying the bath, you can gently massage their tummy with soft, circular motions while they are in the water. This combines the benefits of warmth and massage.
- Post-Bath Comfort: After the bath, wrap your baby in a warm towel, provide plenty of cuddles, and perhaps try a gentle tummy massage again as they dry. The warmth and relaxation might make them more receptive to further gas relief efforts.
Remember, never leave your baby unattended in the bath, even for a second. A warm bath can be a beautiful ritual, bringing comfort and calm to a gassy baby and a stressed parent.
4 Effective Burping Techniques
Burping is often overlooked but is one of the most crucial steps in preventing and relieving baby gas. When babies feed, whether from the breast or a bottle, they inevitably swallow air. If this air isn’t released, it becomes trapped gas, leading to discomfort and fussiness.
The Importance of Burping
Regular burping helps to expel swallowed air before it travels further down the digestive tract and causes pain. It’s not always about a loud burp; sometimes, a small “puff” of air or even a hiccup is enough to indicate success.
Different Burping Positions to Try
Experiment with different positions to find what works best for your baby. Patience is key; sometimes it takes a few minutes for a burp to emerge.
- Over the Shoulder: Hold your baby upright against your chest, with their head resting on your shoulder. Support their head and neck with one hand while gently patting or rubbing their back with the other. The pressure of your shoulder on their belly helps to release air.
- Sitting Upright on Your Lap: Sit your baby on your lap, facing away from you. Support their chest and head with one hand (your palm supporting their chin, fingers supporting their chest, ensuring their airways are clear) and gently pat or rub their back with your other hand. Lean them slightly forward to put gentle pressure on their tummy.
- Face Down on Your Lap: Lay your baby face down across your lap, perpendicular to your body. Their tummy should be resting on your leg, and their head should be slightly higher than their bottom. Support their head with one hand and gently pat or rub their back with the other.
When to Burp:
- During Feeds: For bottle-fed babies, burp them every 2-3 ounces. For breastfed babies, burp them when switching breasts or midway through a long feed.
- After Feeds: Always try to burp your baby after every feeding session, even if they seem asleep.
Tips for Effective Burping:
- Gentle but Firm: Pat or rub your baby’s back gently but with enough firmness to dislodge air bubbles.
- Change Positions: If one position isn’t working, try another.
- Movement: Sometimes a little rocking or jiggling can help.
5 Adjusting Feeding Practices
How your baby feeds can significantly impact the amount of air they swallow, directly influencing their gassiness. Making small adjustments to feeding practices can often bring noticeable relief. This applies whether your baby is breastfed or bottle-fed.
For Breastfed Babies
- Ensure a Good Latch: A proper, deep latch is crucial. When your baby latches well, their mouth covers not just the nipple but also a good portion of the areola, creating a seal that minimizes air intake. If you hear clicking sounds or your baby frequently breaks latch, consult a lactation consultant.
- Upright Feeding Position: Feeding your baby in a more upright position can help milk flow downwards and air rise, making it easier to burp.
- Address Overactive Let-Down: If you have a forceful let-down, your baby might gulp air as they struggle with the fast flow. Try feeding in a laid-back position, or express a little milk before latching your baby.
- Maternal Diet (with caution): While evidence is mixed, some mothers find that certain foods they eat (like dairy, caffeine, cruciferous vegetables) might trigger gas in their breastfed baby. Consider keeping a food diary if you suspect a link, but avoid restrictive diets without professional guidance.
- Emptying the Breast: Ensure your baby empties one breast before offering the other. This helps them get enough hindmilk, which is richer in fat and can aid digestion, potentially leading to less gas than an imbalance of foremilk (which is lighter and more watery).
For Bottle-Fed Babies
- Choose the Right Bottle and Nipple:
- Anti-Colic Bottles: Many bottles are designed with vents or angled shapes to reduce air intake.
- Nipple Flow: Ensure the nipple flow rate is appropriate for your baby’s age and sucking strength. A flow that’s too fast can lead to gulping, while one too slow can cause frustration and air intake.
- Paced Bottle Feeding: Mimic breastfeeding by offering short bursts of feeding followed by pauses. Hold the bottle horizontally, just enough to fill the nipple, allowing your baby to control the flow.
- Upright Feeding Position: Hold your baby in a semi-upright position during bottle feeds, keeping their head higher than their stomach. This helps milk settle below any swallowed air.
- Keep the Nipple Full: Always tilt the bottle so the nipple is completely filled with milk to prevent your baby from sucking in air.
- Burp Frequently: As mentioned, burp your bottle-fed baby every 2-3 ounces to release trapped air proactively.
By carefully observing your baby during feeding and making these simple adjustments, you can often significantly reduce their discomfort from gas.
6 Considering Probiotics and When to Consult Your Doctor
While home remedies are often very effective, sometimes a baby’s gas might be persistent or severe. In such cases, it’s natural to wonder about other options, including supplements like probiotics, and crucially, when it’s time to involve a healthcare professional.
Considering Probiotics for Baby Gas
Probiotics are beneficial bacteria that can help balance the gut microbiome, which plays a vital role in digestion. Some research suggests that certain strains of probiotics, such as Lactobacillus reuteri, may help reduce crying time in colicky, breastfed infants, which often involves significant gas discomfort.
- How They Might Help: Probiotics can potentially improve gut motility, reduce the production of gas-producing bacteria, and aid in the breakdown of lactose, a sugar in milk that some babies struggle to digest.
- Important Caution: Always consult your pediatrician before introducing any supplements, including probiotics, to your baby. They can advise on the appropriate type, dosage, and whether probiotics are suitable for your specific baby’s needs and health history. Self-medicating your infant is never recommended.
- Availability: If recommended by your doctor, baby-specific probiotic drops or powders are available and designed for infant use.
When to Seek Medical Advice
While gas is a normal part of infancy, certain signs warrant a visit to the pediatrician. Trust your parental instincts – if something feels off, it’s always best to get it checked out.
Consult your doctor if your baby exhibits any of the following:
- Persistent, inconsolable crying: Especially if it lasts for hours and isn’t soothed by typical comfort measures.
- Fever: Any fever in a baby under three months old requires immediate medical attention.
- Vomiting: Projectile vomiting or frequent, forceful vomiting.
- Diarrhea or bloody stools: These are signs of a more serious issue.
- Poor weight gain: If your baby isn’t gaining weight as expected.
- Lethargy or extreme fussiness: A significant change in your baby’s demeanor.
- Refusal to feed: If your baby is consistently refusing to eat.
- Severe abdominal distention: A very bloated or hard belly that doesn’t soften.
Your pediatrician can rule out underlying medical conditions, such as allergies, reflux, or more serious digestive issues, and provide tailored advice and treatment options.
A Final Note of Reassurance
Dealing with a gassy baby can be exhausting and emotionally draining, but it’s a phase almost all parents navigate. Remember that you are doing an amazing job, and your baby’s discomfort is not a reflection of your parenting. Be patient with yourself and your little one, try these gentle remedies, and don’t hesitate to reach out to your pediatrician for support. Soon enough, these gassy days will be a distant memory, replaced by countless joyful moments.